Management of Hashimoto’s diseases
> Nutritional depletion and deficiencies
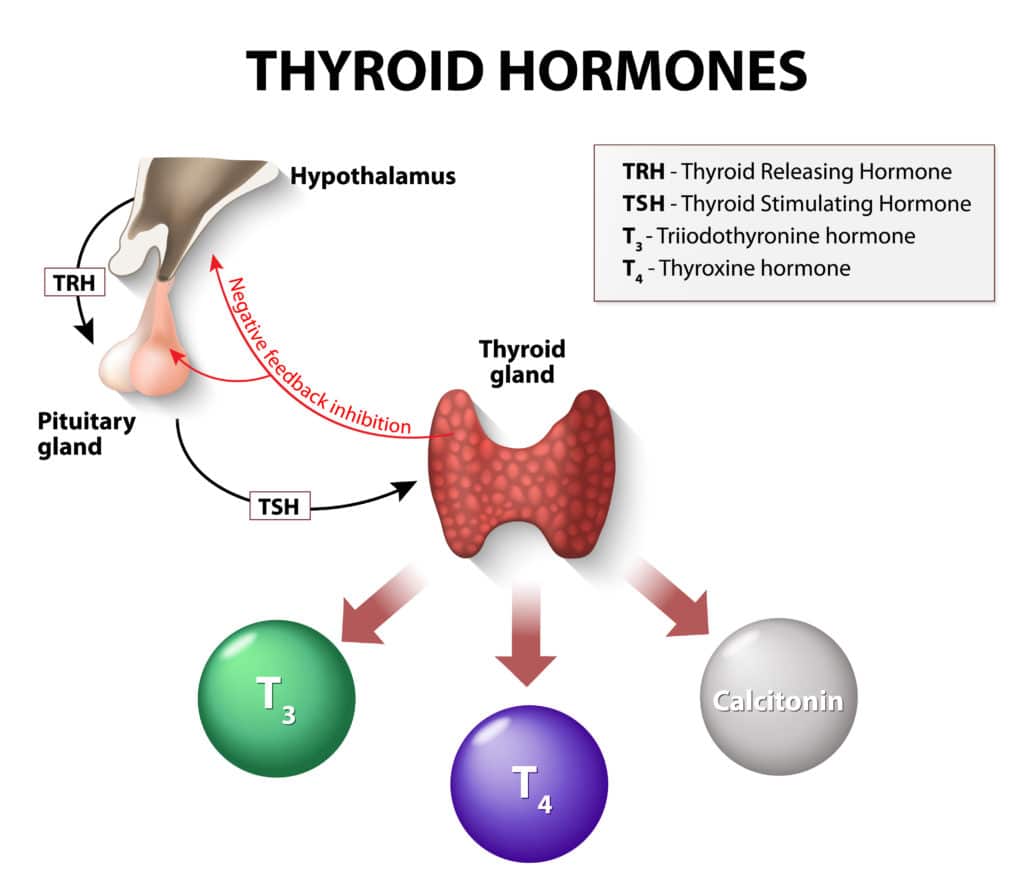
The deficiency of minerals, especially iodine, is linked to abnormal thyroid functions. Including foods rich in iodine or the use of iodine supplements is recommended to promote the secretion of thyroid hormones and restore healthy functioning of the HPT axis.
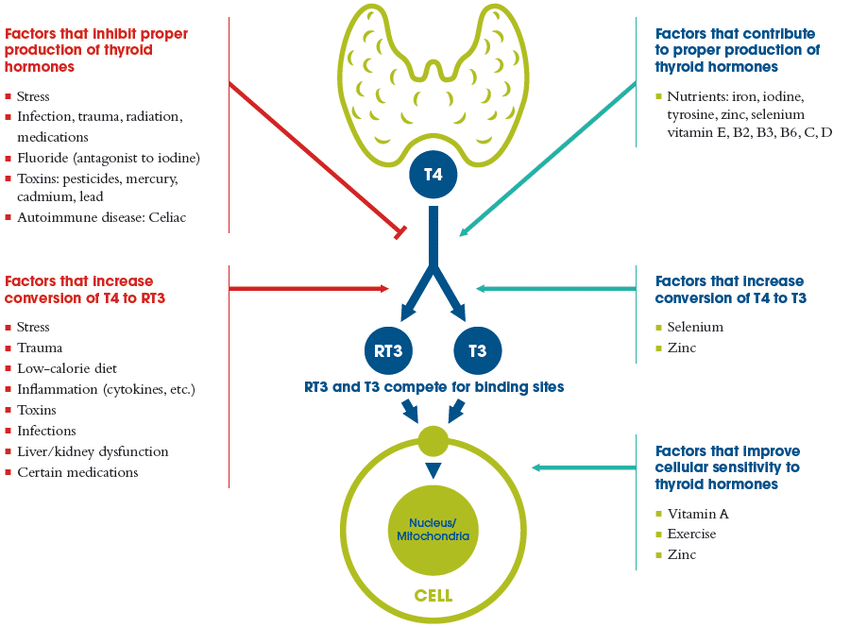
Often, even when someone is eating a nutrient dense, low inflammatory diet there is still the risk of nutritional deficiencies. Factors such as low stomach acid, fat malabsorption and a lack of digestive enzymes will impair the ability to absorb/breakdown nutrients. Common deficiencies include: magnesium, zinc, B vitamins, iron, vitamin D and selenium.
> Inflammation
Chronic inflammation can trigger damage to the healthy tissues of the thyroid and contribute to the faster worsening of the condition. Limiting the consumption of foods containing sugars, sugar substitutes, and unhealthy processed foods is recommended to control inflammation and minimise damage to the gland.
> Food sensitivities
The incidence of Hashimoto’s diseases is higher in patients who suffer from food sensitivities to gluten and dairy. Identifying the specific food sensitivity, you are suffering from and eliminating these foods from the diet could provide faster relief from the symptoms of this disease.
It would also help to reverse damage to the thyroid gland and enable its efficient functioning thereby improving the levels of T3, T4, and TSH.
> Stress and trauma
Mental stress and trauma can not only trigger inflammation but also contribute to adrenal dysfunctions and hormonal disturbances. The stress hormone, cortisol, can directly interfere with thyroid hormone production.
It is advisable to adopt healthy strategies such as meditation and breathing exercises to reduce the effects of mental stress and emotional trauma. It would restore the normal balance of hormones in the nervous system and prevent disruptions in the functions of the hypothalamus, pituitary gland, and thyroid gland.
> Poor sleep and circadian rhythm
Men and women who suffer from insomnia or disturbed sleep due to sleep apnea or restless leg syndrome are more likely to develop Hashimoto’s diseases.
Poor sleep can disrupt the body’s circadian rhythm and worsen hormonal imbalances.
Adopting strategies to improve sleep patterns is expected to improve hormonal balance, reduce mental stress, relieve chronic inflammation, boost immunity, and thus, reverse the damage caused due to Hashimoto’s diseases.
Patients can maintain a fixed sleep-wake routine to improve their circadian rhythm in order to derive relief from thyroid diseases.
> Previous or co-existing infections
Previous or coexisting infections may contribute to inflammation and damage to the thyroid gland. Appropriate treatment of infections, such as ozone therapy can restore the functions of the thyroid within a shorter period.
> Impaired gut health
Impairment of digestive functions due to leaky gut syndrome or poor gut flora can affect immune system functions and trigger the development of autoimmune disorders like Hashimoto’s disease. The most common food sensitives that people react to include certain grains, gluten, dairy and sugar.
Food sensitives are a silent contributor which can exacerbate autoimmune disease, including Hashimoto’s disease.
To support the healing of the gut lining integrity, it is important to remove food sensitivities or food allergens. The use of probiotics could improve gut functions and help to restore healthy activities of the thyroid gland.
> Mitochondrial dysfunctions
Mitochondrial dysfunctions can worsen the symptoms of Hashimoto’s disease by reducing your energy levels and cellular functions.
Improving mitochondrial functions through a nutritious diet is highly recommend to reduce the risk of complications linked to this condition.
> Methylation issue
Analysis of the DNA methylation status in blood cells can provide clues about the possible factors responsible for the development of Hashimoto’s diseases.
Addressing issues related to abnormal methylation can reverse the pathogenesis of this condition and help patients derive relief from the symptoms.
> Obesity and metabolic dysfunctions
Obesity and metabolic dysfunctions like diabetes are known to co-exist in patients with thyroid problems. Blood sugar balance is pivotal for healthy thyroid function (thus often a second autoimmune disease). Individuals who suffer from Hashimoto’s don’t tolerate high sugar/carbs very well as it causes an insulin surge to help clear the extra sugar from the bloodstream. Any major fluctuations or swings in blood sugar levels can actually magnify the symptoms of Hashimoto’s disease.
Maintaining a normal weight, adopting healthy dietary habits, and regular exercises can control these factors and prevent the development of Hashimoto’s disease.
> Toxins & poor detoxification
Exposure to toxins and impaired detoxification pathways can contribute to the accumulation of toxic substances in healthy tissues. Adopting strategies to promote detoxification such as drinking plenty of water every day, taking nutrients to support phase 1 and 2 detox would help to eliminate toxins from your body and restore normal thyroid activities. There are a few environmental toxins found to play a role in Hashimoto’s including but not limited to; synthetic pesticides, polychlorinated biphenyl’s, bisphenol-A, heavy metals, radiotherapy etc.















3 Responses
Very good article! I will add this to Casas de Healing website for educational purpose.
Where can one buy one of those red light things for Thyroid problems; also prices if available
Do you have instructions on useage too? THANKS for helping me.
Hello Shawn, thank you for your comment! Please read this article to learn about the specific options and pricing. https://www.trulyheal.com/red-and-near-infrared-light-a-must-have-therapy/